 Vol.3, No.1, 141-147 (2013) Open Journal of Preventiv e Me dic ine http://dx.doi.org/10.4236/ojpm.2013.31018 Evaluation of a teacher-led physical activity curriculum to increase preschooler physical activity Margaret Dunn-Carver1, Lizzy Pope1*, Gregory Dana2, Anne Dorwald t3, Brian Flynn3, Janice Bunn4, Jean Harvey-Berino1 1Department of Nutrition and Food Sciences, University of Vermont, Burlington, USA; *Corresponding Author: efpope@uvm.edu 2Vermont Child Health Improvement Program, University of Vermont, Burlington, USA 3Office of Health Promotion Research, University of Vermont, Burlington, USA 4Department University Mathematics & Statistics, University of Vermont, Burlington, USA Received 12 January 2013; revised 12 February 2013; accepted 19 February 2013 ABSTRACT Preschool students are generally sedentary at school, and few interventions have addressed whether teacher-led activities can increase physi- cal activity at pr eschools. The cur rent study aimed to increase physical activity in preschool chil- dren enrolled in childcare centers by training childcare providers to deliver a physical activity curriculum. A within-group pre-test/post-test de- sign was used including 32 children at 4 pre- schools. A teacher-led physical activity curricu- lum, the Coordinated Approach to Child Health Early Childhood Education Curriculum (CEC) was implemented in each childcare center for six weeks. Activity levels of participants were monitored through the use of accelerometers and direct observation for approximatel y five hours pre- and post-intervention. Time spent in mod- erate/vigorous physical activity in preschoolers in three of th e four pres chools sugg ested a posi - tive trend increasing from 34.5% ± 13.2% base- line to 39.3% ± 15.4% at follow-up (p = 0.10). Teachers from all four centers reported spend- ing 24.6 ± 13.0 minutes per activity session with up to two activity sessions completed per day. These results justify larger trials to determine the impact of a teacher-led physical activity cur- riculum on the intensity and duration of pre- school students’ physical activity at school. Keywords: Component; Formatting; Style; Styling 1. INTRODUCTION In 2007-2008 10.4% of 2 - 5 years olds were estimated to be obese and 10.8% overweight [1,2]. This trend sig- nifies a national shift toward positive energy balance even in young children [3]. Physical activity is an im- portant contributor to energy balance, and several longi- tudinal studies have demonstrated that physical activity levels are related to weight status in children [4,5]. Addi- tionally, adequate physical activity promotes other posi- tive health outcomes including increased self-esteem, cognitive health, bone formation, overall fitness, and reduced cardiovascular risk factors [6-8]. Furthermore, physical activity behaviors formed during childhood likely persist into adulthood [9-11]. In 2007-2008, 60% or 4.2 million children ages 3 - 5 attended preschools. These environments may play a pivotal role in helping children attain adequate physical activity levels [12,13]. Despite the perception that pre- schoolers are constantly moving during the preschool day, evidence suggests that children in this age group are not getting the recommended amounts of physical activity (PA). Recent studies have revealed that preschoolers typically spend a substantial amount of time (70% - 90% of their day) in sedentary behavior [14-17]. These find- ings suggest that the current level of PA that preschoolers engage in may not meet the recently published Institute of Medicine (IOM) preschool physical activity recom- mendations to prevent early childhood obesity, which suggest providing opportunities for light, moderate, and vigorous physical activity for at least 15 minutes per hour in childcare [18]. Studies have investigated the effectiveness of several physical activity promotion interventions for younger children. These studies employed approaches includ- ing increased recess time, health promotion programs, weight control programs, play equipment, and teacher- guided physical activities in classrooms or on play- grounds [13,19-27]. Several of these studies found posi- tive intervention effects including increased physical activity levels, higher mean heart rate, and more time Copyright © 2013 SciRes. OPEN A CCESS  M. Dunn-Carver et al. / Open Journal of Preventive Medicine 3 (201 3) 141-147 142 spent in vigorous and moderate to vigorous physical ac- tivity (MVPA). Key physical activity promotion targets include physical environment, center policies, staff training, and opportunities for increasing physical activity throughout preschool curricula [28]. Few studies have focused on the association between teacher-guided physical activity and the intensity, duration, and contextual aspects of physical activity [20,21]. Several cross-sectional studies have shown that staff training in physical education is positively associated with children’s physical activity [20,29]. However, to our knowledge, intervention studies have not succeeded in showing a positive effect of a fo- cused teacher training, and subsequent curriculum im- plementation on physical activity of preschool students [28,30]. This study sought to increase physical activity in preschool children enrolled in childcare centers by train- ing childcare providers to deliver a widely available pre- school physical activity curriculum. We hypothesized that a teacher-led, physical activity intervention would increase the time and intensity of preschool children’s physical activity. 2. METHODS 2.1. Participants The study was conducted within preschool classrooms at four licensed childcare centers in Vermont. Potential centers were selected with consideration of the number of children available in the targeted 4 - 5 years age group, the amount of space available to feasibly implement the intervention program activities, absence of a significant physical activity asset such as a gym at the facility, and diversity of the populations served. Enrollment of centers occurred from December 2009 to January 2010. All children ages 4 - 5 attending the enrolled centers were eligible for the study. Center staff provided consent forms and letters describing the study and data collection procedures to parents of 4 - 5 year-old children. Centers were offered an incentive of $400 for participation, in addition to staff training and equipment needed to im- plement the curriculum. Thirty-two children participated in the study. 2.2. Instruments Measures used to document impact, implementation, and acceptability of the CEC program included objective measures of physical activity, observer reports, and logs and surveys provided by participating teachers. Physical Activity Measurement. Children’s physical activity was measured with a SenseWear®Pro 3 armband (BodyMedia, Pittsburgh, PA) (SWA) during the baseline and follow-up periods. SWA assessed physical activity levels over time as average metabolic equivalent of task (MET) per minute. The device is worn on the triceps of the upper right arm and held in place by a Velcro arm- band strap. It uses a combination of five sensors, includ- ing a two-axis accelerometer, plus participant’s height, weight, and age to calculate total energy expenditure, active energy expenditure, average MET levels, number of steps, and sleep and lying down duration for each minute of use. The SWA has been tested in a variety of adult populations and has been validated in resting state, during exercise, and in obese individuals [31]. Further- more, recent studies by Calabro et al. showed that SWAs validly assess physical activity in children [32,33]. The output of interest for this study was physical activity by MET levels: sedentary (≤1.4 METs), light (1.5 - 2.9), moderate (>3 to 5.9 METs), and vigorous (≥6 METs) [34]. Direct Observation of Children’s Activities. Trained study staff conducted direct observations recording a sequence of activity categories for individual children delimited by specific times that could be linked with minute-by-minute accelerometer measures of activity levels for the same children over these time periods. Ob- servers recorded a brief description of each of the 4-5 children they were following on a structured form. Ob- servers then recorded the time each new type of activity began throughout the observation period. Observers also indicated whether the activity was indoors or outdoors, and whether the activity was a teacher-guided activity or free-play activity. After the observation session, each activity was further categorized by additional codes in- dicating whether the activity was free play with a gross motor emphasis (FGM), teacher-led gross motor (TGM) play, or manipulative, sedentary, sedentary with limb movement, transitional, or unique activity. These catego- ries were adapted from Brown et al [35]. A review by Pate et al. indicated that both direct observation systems and accelerometry are well established, valid, reliable, and complimentary measures of physical activity in young children [36]. Height and Weight. Anthropometric measures were taken on the first day of baseline measurements with children wearing street clothes and without shoes. Re- search staff used a calibrated floor scale (Tanita, BWB- 800A) to measure weight; height was measured using a wall-mounted tape measure with square on head. Body Mass Index (BMI) was calculated as weight (kg)/height (m2) and BMI-for-age percentile was calculated using standard growth charts [37]. Teacher Logs and Post-Intervention Surveys. Partici- pating teachers completed daily logs of CEC lessons used and lesson duration during the 6-week curriculum implementation. They indicated how closely the activi- ties were followed using a scale where 1 = not at all and 4 = completely. Children’s level of enthusiasm in re- Copyright © 2013 SciRes. OPEN A CCESS  M. Dunn-Carver et al. / Open Journal of Preventive Medicine 3 (201 3) 141-147 143 sponse to the activities was recorded using a scale where 1 = not at all enthusiastic and 5 = extremely enthusiastic. Teachers also were asked to complete a semi-structured post-intervention survey regarding the acceptability and ease of implementation of the CEC curriculum. Observer Reports. A physical education teacher and a research staff member visited participating classrooms 2 - 3 weeks into the intervention period to observe whether the CEC activities were being implemented as intended. Observations occurred for one half day in each center, and observer reports were filled out using a form adapted from CEC evaluation materials. 2.3. Procedure This 10-week study used a pre-test/post-test design. Baseline measures were conducted in February/March 2010, a six-week intervention occurred, and follow-up measures were conducted in April/May 2010. In both the baseline and follow-up periods assessments of partici- pating children’s physical activity levels were completed over two consecutive mornings at the childcare center. Teachers attended a one-day training on the Coordinated Approach to Child Health (CATCH) elementary educa- tion program and then implemented the curriculum for six weeks, keeping logs of the components implement- ed. The CATCH Early Childhood Curriculum (CEC) is based on the grades 3 - 5 Coordinated Approach to Child Health (CATCH) elementary education program [38]. The CATCH program uses Social Cognitive Theory as a foundation for the design of activities to promote posi- tive changes in multiple health behaviors, including physical activity. Preliminary evaluations of the CEC program demonstrated feasibility and acceptability among children, teachers and parents [39]. This study focused on the CEC physical activity components aimed at in- creasing moderate to vigorous physical activity (MVPA) through classroom activities enhanced with play equip- ment, and stimulated by music and group games. Table 1 provides a description of activity categories and example activities. Seven teachers from the four centers participated in a one-day CEC curriculum training conducted by a CATCH/ CEC National Training Staff member. Each center re- ceived the CEC physical education curriculum kit and accompanying equipment. Participating teachers were asked to implement at least two CEC curriculum activity sessions per day during the six-week intervention period (~60 minutes per day). There was no additional supervi- sion during this period. 2.4. Data Analysis Data from the SWAs were downloaded into individual Table 1. CATCH early childhood activity categories. I. Warm-up Short 3 - 5 minutes activities designed to prepare for more vigorous movement II. Go Fitness Intended to promote muscular strength, muscular endurance, and cardiovascular endurance III. Go Activity Activities that develop fundamental motor skills and rhythm IV. Limber Limbs Purposeful movement to improve muscular range of motion such as stretching and twisting V. Cool Down Cool down students' bodies and help with transition back to the classroom files for each participant for each observation session. Data were analyzed using Inner View Research Software (version 6.1) provided by the SWA manufacturer. Ob- servation data (e.g., indoor/outdoor, guided/free play) was hand coded and linked by time stamp to SWA data. Continuous variables are reported as means ± standard deviations; categorical variables are reported as frequen- cies and percentages. The analytic approach was a sin- gle-group repeated measures analysis of variance. For analysis of baseline-to-follow up intervention changes, time point was considered a fixed effect, with random variables included to account for the correlation among repeated measures taken on the same child as well as the correlation among children clustered within a preschool program. These analyses included only those children with data collected in both time points. All analyses were performed using SAS, version 9.2 (SAS Institute Inc., 2002). 3. RESULTS 3.1. Participant Descriptors Of 46 children with signed parental consent forms, 42 (91%) participated in the study. Among these children, 32 (76%) completed both baseline and follow-up meas- ures. The mean age of participating children was 4.3 ± 1.5 (range: 4 - 5) years; 46.3% were male. Participants had an average BMI of 15.9 kg/m2 ± 1.1; 2.4% were obese, and 12.2% were overweight. A completer versus non-completer analysis revealed no significant differ- ences in age, gender, BMI, or baseline activity levels between children who completed all measures and those who did not. Therefore, analysis focused on children completing both baseline and follow-up measures (n = 32). Reasons why consented children did not complete the assessments included temporary absence and leaving the preschool program. Seven preschool teachers from the four centers participated in the CEC training, imple- mented the program in their classrooms, and completed a survey assessment of the curriculum at the end of the follow-up period. Five of these teachers logged the fre- quency, duration, and type of each CEC activity imple- mented. Copyright © 2013 SciRes. OPEN A CCESS 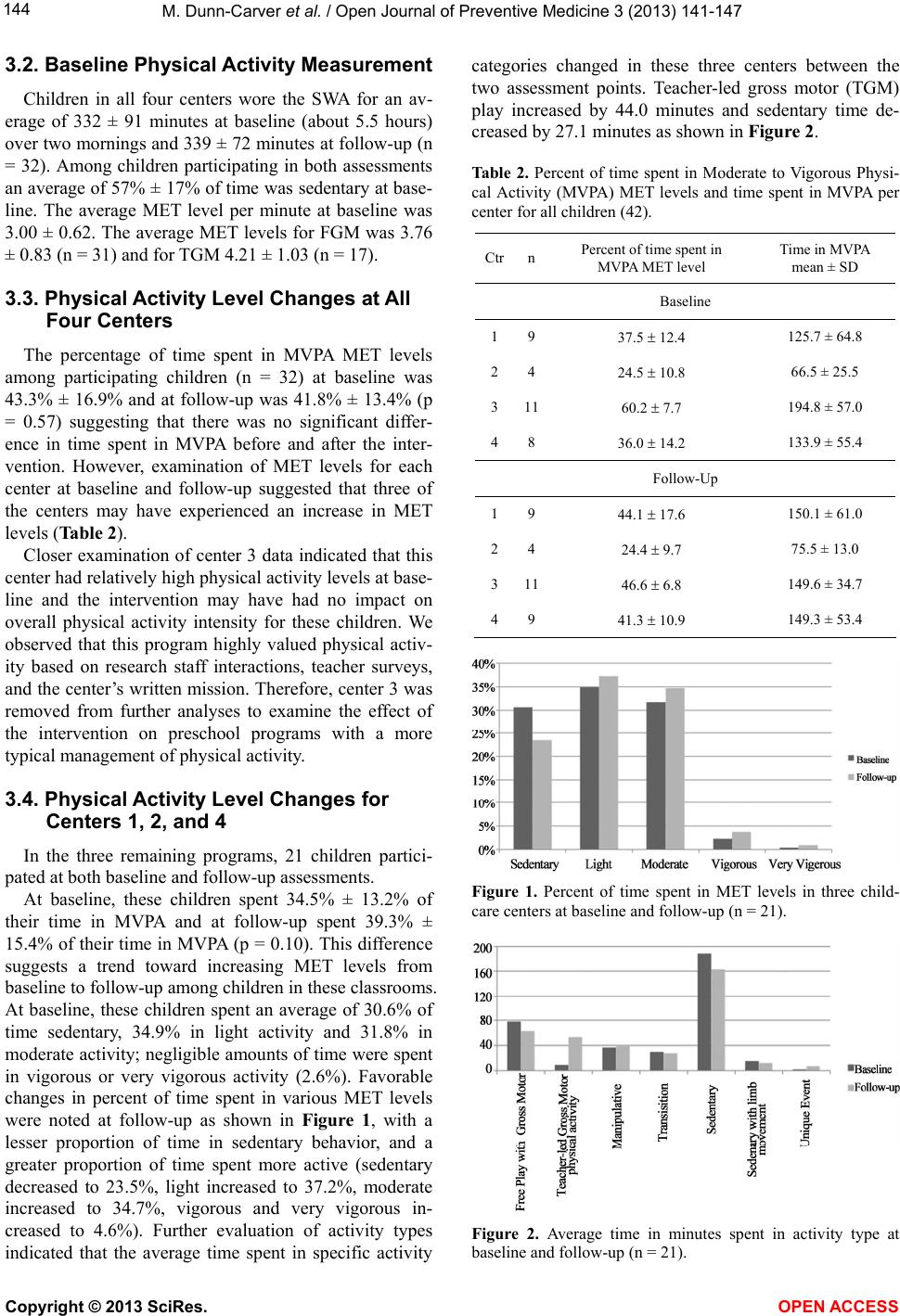 M. Dunn-Carver et al. / Open Journal of Preventive Medicine 3 (201 3) 141-147 144 3.2. Baseline Phys ical Activity Measurement Children in all four centers wore the SWA for an av- erage of 332 ± 91 minutes at baseline (about 5.5 hours) over two mornings and 339 ± 72 minutes at follow-up (n = 32). Among children participating in both assessments an average of 57% ± 17% of time was sedentary at base- line. The average MET level per minute at baseline was 3.00 ± 0.62. The average MET levels for FGM was 3.76 ± 0.83 (n = 31) and for TGM 4.21 ± 1.03 (n = 17). 3.3. Physical Activity Level Changes at All Four Centers The percentage of time spent in MVPA MET levels among participating children (n = 32) at baseline was 43.3% ± 16.9% and at follow-up was 41.8% ± 13.4% (p = 0.57) suggesting that there was no significant differ- ence in time spent in MVPA before and after the inter- vention. However, examination of MET levels for each center at baseline and follow-up suggested that three of the centers may have experienced an increase in MET levels (Table 2). Closer examination of center 3 data indicated that this center had relatively high physical activity levels at base- line and the intervention may have had no impact on overall physical activity intensity for these children. We observed that this program highly valued physical activ- ity based on research staff interactions, teacher surveys, and the center’s written mission. Therefore, center 3 was removed from further analyses to examine the effect of the intervention on preschool programs with a more typical management of physical activity. 3.4. Physical Activity Level Changes for Centers 1, 2, and 4 In the three remaining programs, 21 children partici- pated at both baseline and follow-up assessments. At baseline, these children spent 34.5% ± 13.2% of their time in MVPA and at follow-up spent 39.3% ± 15.4% of their time in MVPA (p = 0.10). This difference suggests a trend toward increasing MET levels from baseline to follow-up among children in these classrooms. At baseline, these children spent an average of 30.6% of time sedentary, 34.9% in light activity and 31.8% in moderate activity; negligible amounts of time were spent in vigorous or very vigorous activity (2.6%). Favorable changes in percent of time spent in various MET levels were noted at follow-up as shown in Figure 1, with a lesser proportion of time in sedentary behavior, and a greater proportion of time spent more active (sedentary decreased to 23.5%, light increased to 37.2%, moderate increased to 34.7%, vigorous and very vigorous in- creased to 4.6%). Further evaluation of activity types indicated that the average time spent in specific activity categories changed in these three centers between the two assessment points. Teacher-led gross motor (TGM) play increased by 44.0 minutes and sedentary time de- creased by 27.1 minutes as shown in Figure 2. Ta ble 2. Percent of time spent in Moderate to Vigorous Physi- cal Activity (MVPA) MET levels and time spent in MVPA per center for all children (42). Ctr nPercent of time spent in MVPA MET level Time in MVPA mean ± SD Baseline 1 937.5 12.4 125.7 ± 64.8 2 424.5 10.8 66.5 ± 25.5 3 1160.2 7.7 194.8 ± 57.0 4 836.0 14.2 133.9 ± 55.4 Follow-Up 1 944.1 17.6 150.1 ± 61.0 2 424.4 9.7 75.5 ± 13.0 3 1146.6 6.8 149.6 ± 34.7 4 941.3 10.9 149.3 ± 53.4 Figure 1. Percent of time spent in MET levels in three child- care centers at baseline and follow-up (n = 21). Figure 2. Average time in minutes spent in activity type at baseline and follow-up (n = 21). Copyright © 2013 SciRes. OPEN A CCESS  M. Dunn-Carver et al. / Open Journal of Preventive Medicine 3 (201 3) 141-147 145 3.5. Teacher and Observer Reports Teachers from all four centers reported spending 24.6 ± 13.0 minutes per CEC session with up to two sessions completed per day. Center 2 reported at least one CEC session over all 30 days; center 1 and 4 missed one day of CEC sessions; center 3 did not complete any sessions on 11 days. Teachers reported following the curriculum closely (3.15 where 1 = not at all and 4 = completely) and indicated that the children were generally enthusias- tic (3.94 where 1 = not enthusiastic and 5 = very enthu- siastic) about the program. Two independent observers also reported that children actively participated in the activities, which were conducted as designed. 4. DISCUSSION The overall findings suggest that using a physical ac- tivity curriculum may be a feasible and effective ap- proach to increasing physical activity among preschool students. During six weeks of implementing CEC, teach- ers logged at least 25 minutes of recommended activities per day and reported high levels of enthusiasm by the students. Independent observers reported high levels of participation by the children and the staff. In three child- care centers with lower baseline levels of physical activ- ity, positive trends towards greater amounts of time in MVPA were observed. More specifically, child participa- tion in teacher-led gross motor activities appeared to in- crease following implementation of the curriculum in these three centers, as intended by the CEC design. As- sessments of children in one center that had higher base- line levels of MVPA did not reflect these positive trends, however. On average during the baseline period, all four centers were sedentary or engaged in light activity for more than 50% of the observation time, and less than one percent of the time was spent in vigorous or very vigorous activity. When center three was removed from the analyses, we discovered that the centers spent on average almost 70% of the preschool day in sedentary or light behavior. In order to meet IOM guidelines recommending that chil- dren get at least 15 minutes of physical activity per hour, we requested that teachers incorporate at least two ses- sions of CEC per day. Unfortunately, most teachers did not meet this goal. This deficit may be explained by the challenge that teachers faced in engaging the children for the recommended structured physical activity time. Also, decreased ability to engage in active play may have re- sulted from space limitations in the childcare centers, an important environmental determinant of physical activity for children attending childcare [13,20]. This study adds to the small amount of research fo- cused on physical activity curriculum interventions for preschoolers. Use of multiple methods of evaluation to assess the context, duration, acceptability, feasibility, and intensity of physical activity during the school day is a strength of the study. This is the first study to use a multi-sensor armband accelerometer to quantify the im- pact of a physical activity curriculum on physical activity levels attained during the preschool day. The physical activity program was delivered by the usual preschool teaching staff rather than research staff or outside profes- sionals, highlighting the potential of a one-day teacher training as a means to increase physical activity in pre- school students. Limitations There were several limitations to this study. The study employed a within-group design, and therefore did not have a control group to account for the influence of secular or seasonal trends in activity. The sample size was small, limiting our ability to detect differences be- tween baseline and follow-up measurements as statisti- cally significant. Loss during follow up contributed to this limitation although it may be typical for this popula- tion. Another limitation was the short duration, as an average of five hours of observation per child over a lim- ited time frame may not be sufficient to observe other factors that influence preschool physical activity. This study drew from a convenience sample population that may limit generalizability. Finally, although we did not collect ethnic or racial information, we are aware that overall the Vermont ethnic/race distribution is largely homogeneous which could also limit generalizability; it should be noted, however, that the CEC was developed in settings with more diverse populations. 5. CONCLUSION Considering the detrimental health implications of a sedentary lifestyle for children and the rise in childhood obesity, activity at childcare centers remains a critical area of research. In fact, this area of research has been recognized as being increasingly important by the June 2011 IOM report suggesting that childcare regulatory agencies require that childcare providers engage pre- school children in physical activity throughout the day [18]. The positive trends in MVPA among 4 - 5 years old at childcare centers found in this study suggest that a focused physical activity curriculum may be an effective way to increase activity during the preschool day. Addi- tionally, preschool teachers reported a high level of sat- isfaction and efficacy in implementing the CEC program and perceived their students to be enthusiastic about the program. These results suggest that larger trials may be justified to provide stronger evidence for the impact of a CEC curriculum on the intensity and duration of pre- school students’ physical activity in childcare settings. Copyright © 2013 SciRes. OPEN A CCESS  M. Dunn-Carver et al. / Open Journal of Preventive Medicine 3 (201 3) 141-147 146 6. ACKNOWLEDGEMENTS The authors are grateful to the participating preschools, directors, providers, children and their parents who invested their time in the study. We would also like to acknowledge all members of the project team not listed as authors and Dr. David Brock for his valuable input. This work was supported by grant NIFA #2008-04099 from the US Department of Agriculture awarded to Jean Harvey-Berino, R.D., Ph.D. REFERENCES [1] Ogden, C., Carroll, M., Curtin, L., Lamb, M. and Flegal, K. (2010) Prevalence of high body mass index in US children and adolescents, 2007-2008. Jama, 303, 242. doi:10.1001/jama.2009.2012 [2] Kim, J., Peterson, K., Scanlon, K., Fitzmaurice, G., Must, A., Oken, E., Rifas-Shiman, S., Rich-Edwards, J. and Gill- man, M. (2006) Trends in Overweight from 1980 through 2001 among preschool-aged children enrolled in a Health Maintenance Organization. Obesity, 14, 1107-1112. doi:10.1038/oby.2006.126 [3] Troiano, R. and Flegal, K. (1998) Overweight children and adolescents: Description, epidemiology, and demo- graphics. Pediatrics, 101, 497. [4] Jago, R., Baranowski, T., Baranowski, J., Thompson, D., and Greaves, K. (2005) BMI from 3-6 y of age is pre- dicted by TV viewing and physical activity, not diet. In- ternational Journal of Obesity, 29, 557-564. doi:10.1038/sj.ijo.0802969 [5] Moore, L., Gao, D., Bradlee, M., Cupples, L., Sundara- jan-Ramamurti, A., Proctor, M., Hood, M., Singer, M. and Ellison, R. (2003) Does early physical activity predict body fat change throughout childhood? Preventive Medi- cine, 37, 10-17. doi:10.1016/S0091-7435(03)00048-3 [6] Fulton, J., Garg, M., Galuska, D., Rattay, K. and Casper- sen C. (2004) Public health and clinical recommendations for physical activity and physical fitness: Special focus on overweight youth. Sports Medicine, 34, 581-599. doi:10.2165/00007256-200434090-00003 [7] Baranowski, T., Mendlein, J., Resnicow, K., Frank, E., Cullen, K.W. and Baranowski, J. (2000) Physical Activity and Nutrition in Children and Youth: An Overview of Obesity Prevention. Preventive Medicine, 31, S1-S10. doi:10.1006/pmed.2000.0686 [8] Hillman, C., Erickson, K. and Kramer. A. (2008) Be smart, exercise your heart: Exercise effects on brain and cognition. Nature Reviews Neuroscience, 9, 58-65. doi:10.1038/nrn2298 [9] Bandura, A. (2004) Health promotion by social cognitive means. Health Education & Behavior, 31, 143. doi:10.1177/1090198104263660 [10] Birch, L. and Fisher, J. (1998) Development of eating behaviors among children and adolescents. Pediatrics, 101, 539. [11] Telama, R., Yang, X., Viikari, J., Wanne, I.O. and Raita- kari, O. (2005) Physical activity from childhood to adult- hood: A 21-year tracking study. American Journal of Pre- ventive Medicine, 28, 267-273. doi:10.1016/j.amepre.2004.12.003 [12] (2009) America’s children: Key national indicators of well-being. http://www.childstats.gov/americaschildren/famsoc3.asp [13] Dowda, M., Brown, W., McIver, K., Pfeiffer, K., O’Neill, J., Addy, C. and Pate, R. (2009) Policies and characteris- tics of the preschool environment and physical activity of young children. Pediatrics, 123, e261. doi:10.1542/peds.2008-2498 [14] Reilly, J. (2010) Low levels of objectively measured physical activity in preschoolers in childcare. Medicine & Science in Sports & Exercise, 42, 502-507. doi:10.1249/MSS.0b013e3181cea100 [15] Brown, W.H., Googe, H.S., McIver, K.L. and Rathel, J.M. (2009) Effects of teacher-encouraged physical activity on preschool playgrounds. Journal of Early Intervention, 31, 126-145. doi:10.1177/1053815109331858 [16] Pate, R., McIver, K., Dowda, M., Brown, W. and Addy, C. (2008) Directly observed physical activity levels in pre- school children. Journal of School Health, 78, 438-444. doi:10.1111/j.1746-1561.2008.00327.x [17] Reilly, J. (2008) Physical activity, sedentary behaviour and energy balance in the preschool child: Opportunities for early obesity prevention, Proceedings of the Nutrition Society, 67, 317-325. doi:10.1017/S0029665108008604 [18] Institute of Medicine of the National Acedmies (2011) Early childhood obesity prevention policies. Washington DC. [19] Hannon, J. and Brown, B. (2008) Increasing preschool- ers’ physical activity intensities: An activity-friendly pre- school playground intervention. Preventive Medicine, 46, 532-536. doi:10.1016/j.ypmed.2008.01.006 [20] Bower, J., Hales, D., Tate, D., Rubin, D., Benjamin, S. and Ward, D. (2008) The childcare environment and chil- dren’s physical activity. American Journal of Preventive Medicine, 34, 23-29. doi:10.1016/j.amepre.2007.09.022 [21] Parish, L., Rudisill, M. and St Onge, P. (2007) Mastery motivational climate: Influence on physical play and heart rate in African American toddlers. Research Quar- terly for Exercise & Sport, 78, 171-178. doi:10.5641/193250307X13082490460823 [22] Alhassan, S., Sirard, J. and Robinson, T. (2007) The ef- fects of increasing outdoor play time on physical activity in Latino preschool children. International Journal of Pediatric Obesity, 2, 153-158. doi:10.1080/17477160701520108 [23] Binkley, T. and Specker, B. (2004) Increased periosteal circumference remains present 12 months after an exer- cise intervention in preschool children. Bone, 35, 1383- 1388. doi:10.1016/j.bone.2004.08.012 [24] Eliakim, A., Nemet, D., Balakirski, Y. and Epstein, Y. (2007) The effects of nutritional-physical activity school- based intervention on fatness and fitness in preschool children. Journal of Pediatric Endocrinology & Metabo- lism, 20, 711-718. [25] Fitzgibbon, M., Stolley, M., Schiffer, L., Van Horn, L., Kaufer, C.K. and Dyer, A. (2005) Two-year follow-up results for hip-hop to health Jr.: A randomized controlled Copyright © 2013 SciRes. OPEN A CCESS  M. Dunn-Carver et al. / Open Journal of Preventive Medicine 3 (201 3) 141-147 Copyright © 2013 SciRes. OPEN A CCESS 147 trial for overweight prevention in preschool minority children. The Journal of pediatrics, 146, 618-625. doi:10.1016/j.jpeds.2004.12.019 [26] Reilly, J., Kelly, L., Montgomery, C., Williamson, A., Fisher, A. McColl, J., Lo Conte, R., Paton J. and Grant, S. (2006) Physical activity to prevent obesity in young chil- dren: Cluster randomized controlled trial. British Medical Journal, 333, 1041. doi:10.1136/bmj.38979.623773.55 [27] Trost, S., Fees, B. and Dzewaltowski, D. (2008) Feasibil- ity and efficacy of a “move and learn” physical activity curriculum in preschool children. Journal of Physical Ac- tivity & Health, 5, 88. [28] Ward, D., Vaughn, A., McWilliams, C. and Hales, D. (2009) Physical activity at child care settings: Review and Research recommendations. American Journal of Life- style Medicine, 3, 474. doi:10.1177/1559827609341964 [29] Dowda, M., Pate, R., Trost, S., Almeida, M. and Sirard, J. (2004) Influences of preschool policies and practices on children’s physical activity. Journal of Community Health, 29, 183-196. doi:10.1023/B:JOHE.0000022025.77294.af [30] Reilly, J. and McDowell, Z. (2003) Physical activity in- terventions in the prevention and treatment of paediatric obesity: Systematic review and critical appraisal. Pro- ceedings of the Nutrition Society, 62, 611-619. doi:10.1079/PNS2003276 [31] Papazoglou, D., Augello, G., Tagliaferri, M., Savia, G., Marzullo, P., Maltezos, E. and Liuzzi, A. (2006) Evalua- tion of a multisensor armband in estimating energy ex- penditure in obese individuals. Obesity, 14, 2217-2223. doi:10.1038/oby.2006.260 [32] Calabro, M., Welk, G. and Eisenmann, J. (2009) Valida- tion of the sensewear pro armband algorithms in children. Medicine and Science in Sports and Exercise, 41, 1714. doi:10.1249/01.MSS.0000355193.19476.d5 [33] Calabro, M.A., Lee, J., De St-Maorice, P. and Welk, G.J. (2011) Validation of pattern-recognition monitors in chil- dren using doubly-labeled water. in American College of Sports Medicine Conference, 43, 132. doi:10.1249/01.MSS.0000403068.22614.ab [34] Pate, R., Pfeiffer, K., Trost, S., Ziegler, P. and Dowda, M. (2004) Physical activity among children attending pre- schools. Pediatrics, 11 4, 1258-1263. doi:10.1542/peds.2003-1088-L [35] Brown, W., Pfeiffer, K., Mclever, K., Dowda, M., Almeida, M. and Pate, R. (2006) Assessing preschool children’s physical activity: The observational system for recording physical activity in children-preschool version. Research Quarterly for Exercise and Sport, 77, 167-176. doi:10.5641/027013606X13080769704361 [36] Pate, R., O’Neill, J. and Mitchell, J. (2010) Measurement of physical activity in preschool children. Medicine & Science in Sports & Exercise, 42, 508-512. doi:10.1249/MSS.0b013e3181cea116 [37] Kuczmarski, R., Ogden, C., Grummer-Strawn, L., Flegal, K., Guo, S., Wei, R., Mei, Z., Curtin, L., Roche, A. and Johnson, C. (2000) CDC growth charts: United States. Advance Data, 314, 1-27. [38] Stone, E., McKenzie, T., Welk, G. and Booth, M. (1998) Effects of physical activity interventions in youth. Ameri- can Journal of Preventive Medicine, 15, 298-315. doi:10.1016/S0749-3797(98)00082-8 [39] Sharma, S., Chuang, R.J. and Hedberg, A.M. (2011) Pilot testing CATCH early childhood: A preschool-based pro- gram aimed at promoting healthy nutrition and physical activity among 3 to 5 year old children enrolled in head start. American Journal of Health Education, 42, 12-23. doi:10.1080/19325037.2011.10599169
|