Epidemiological Studies on the Relationship between PTSD Symptoms and Circadian Typology and Mental/Sleep Health of Young People Who Suffered a Natural Disaster, Great Hanshin-Awaji Earthquake ()
1. Introduction
1.1. Disasters and PTSD
On 17th January 1995, the Great Hanshin-Awaji earthquake with a magnitude of 7.2 as the Richter scale attacked Hanshin-Awaji area in Japan. The earthquake killed 6434 people [1] . Many studies investigating the psychological states of natural disaster victims, especially earthquakes such as in Italy [2] , Armenia [3] , and China [4] , have been demonstrated. Kato et al. [5] assessed the frequency of short-term, post-traumatic symptoms among survivors of the Hanshin-Awaji earthquake using the Post-Traumatic Symptom Scale. This paper reported that subjects experienced sleep disturbances, depression, hypersensitivity, and irritability during the third week after the earthquake.
Three and half years after a severe earthquake (7.3 on the Richter scale) in Taiwan, the estimated rate of survivors with posttraumatic stress symptoms (PTSS) was 23.8% and 4.4%, respectively, and PTSS scores were highly correlated with QOL scores (less severe symptoms with higher QOL) [6] . Even 4 years after the Parnitha earthquake in Greece, 22% of survivors reported subjective distress and intense fear during the earthquake, and participation in rescue operations positively correlated with greater post-earthquake psychological stress [7] . The psychological consequence of earthquakes may be serious and long-lasting even when the magnitude of the earthquake is moderate [7] .
1.2. Circadian Typology and Sleep Habits
The ongoing 24-hour commercialization society accelerated shifting to evening-typed life for many people [8] . As a result, 24-hour commercialization society may reduce the amplitudes of environmental daily cycles of light, social activities, and food intake. Persistent lower amplitudes of several zeitgebers may induce an inner-desynchronized protocol between the main clock, which drives the autonomous nervous system, and the slave clock, which controls the sleep-wake cycle (Double-oscillations theory [9] ). So, evening-typed diurnal rhythms, which are linked to the shortage of sleep due to late bedtimes and also poor quality of sleep [10] -[15] , may lead to lower moods and higher levels of irritation than morning-typed ones [16] .
1.3. PTSD, Sleep Disturbance and Circadian Typology
A previous study to assess the quality of sleep and its architecture in injured victims of traffic accidents one year after the accident found that the problem in PTSD is mainly sleep misperception rather than actual sleep alteration [17] . On the other hand, Wang et al. [18] reported that sleep disturbance is one of 4 factors indicating PTSD symptoms as assessed by the Impact Event Scale-Revised (IES-R) and the main symptom exhibited in PTSD. Some studies were consistent [19] [20] .
Another previous study aimed to determine the relationship between Post Traumatic Stress Disorder (PTSD) and current circadian typology and sleep habits of adults who experienced the Great Hanshin-Awaji Earthquake after becoming adults [21] . Kuroda et al. [21] found that people who damaged strongly from a disaster and who currently show severe PTSD symptoms are more evening-typed and have a lower quality of sleep. However, whether PTSD symptoms of young people who suffered the Hanshin-Awaji earthquake in childhood can be reduced by the morning-typed life was remained to be studied.
This study aims, first, to determine the relationship between Post Traumatic Stress Disorder (PTSD) and current circadian typology and sleep habits of people who experienced the Great Hanshin-Awaji Earthquake in their childhood in January 1995. The second aim is to evaluate the effects of an intervention on sleep and mental health including PTSD symptoms of such young participants using a leaflet on “Go to bed early, Get up early and Do not forget to have a breakfast” and a sleep diary.
2. Participants and Methods
2.1. Questionnaire Study
An integrated questionnaire was administered to 275 people aged 19 - 37 years old (mean age: 21.9 years) in Hyogo Prefecture (35˚N), Japan in March 2012, with responses received from 275 people (females: 173, males: 93, unknown: 9) which were all available for analysis. The questionnaire consisted of basic questions about attributes such as age and sex, questions on sleep habits and sleep quality, the Torsvall-Åkerstedt Diurnal Type Scale [22] and a Japanese version [23] of the Impact of Event Scale-Revised (IES-R) which has been usually used as PTSD scores [24] composed of 22 questions, 8 questions related to “intrusion”, 6 on “hyper-arousal” and 8 on “avoidance-numbing”. The original questions on sleep habits which Harada et al. [25] originally constructed have been used in several papers [26] -[31] .
2.1.1. Statistical Analysis
The data was statistically analyzed using Mann-Whitney U-tests and Pearson’s correlation analysis with SPSS 20.0 statistical software. Diurnal Type scale scores were expressed as means plus or minus the standard deviation (Mean ± SD).
2.1.2. Criterion for High and Low Damage Groups
Participants were divided into a High Damage Group (HDG) and a Low Damage Group (LDG) based on the IES-R scores. Participants who scored 25 or more in the IES-R were placed in HDG and those who scored less than 25 were placed in LDG.
2.2. Intervention Study
An intervention program using a leaflet to promote the morning-typed life for persons who suffered natural disaster, entitled “Go to bed early, Get up early and Do not forget to have a breakfast, for getting three benefits!”. Participants were asked to follow the 5 contents of intervention, included in the leaflet.
The intervention program was administered to 96 participants belonging to school of nursing. To estimate the effects of the one month intervention, integrated questionnaires were administered to all participants two times: before the start of the intervention period and one or two months after the end of the intervention period (See legend of Figure 1). Ninety-four of 96 (98%) participants answered the first questionnaire and 72 of 94 (77%) kept sleep diaries for 21 days and answered the second questionnaire. Participants aged 38 or more were eliminated. Finally 66 participants (male: 7, female: 57, unclear: 2, 19 - 37 years old, average age: 22.73) were used for analysis.
All participants were asked to keep a sleep diary throughout the 21 days of the intervention period, which was in November or December of 2012. To counterbalance the effect of the day length, two intervention periods were set across the winter solstice. Twenty-three subjects participated in the intervention in November and 43 participants did in December. The sleep diary consisted of questions on sleep habits (including falling asleep time and awakening time), physical condition, mood on awakening, awakening frequency during night sleep, and the implementation status of 5 contents of intervention (Table 1).
Participants marked their implementation status every day. For the 1st and 3rd contents, they marked circle or × for “Yes” or “No” and answered how many minutes they had been exposed to sunlight. For the 2nd content, they chose one from four choices for breakfast contents (a double circles: they had nutritionally well balanced breakfast; a circle: they had breakfast including staple diet; a triangle: they had something; a ×-marking: they had nothing). For the 4th content, they marked a circle when they had not watched the TV program. If they had watched it on TV, they did a ×-marking and filled how many minutes they had watched. For the 5th content, they filled how many hours they had stayed under fluorescent light.
For the statistical analysis, the “implementation score” was calculated. A circle of the 1st, 3rd, and 4th contents

Figure 1. Schedule of the intervention study.

Table 1. 5 contents of intervention in the leaflet.
meant 1 point and a ×-mark was 0 point. A double circle of the 2nd content was 1 point, a circle was 0.67 points, a triangle was 0.33 points, and a ×-mark did 0 points. On the 5th content, “0 hour” converted to 1 point and “the maximum hours” among all participants each day converted to 0 point. The other hours were rationally converted to the mark distributed from 0 and 1 points, in each day.
The 21-day-long intervention period was divided into 3 parts (FWP: First week period, MWP: Middle week period, LWP: Last week period). The “high implementation group (HIG)” was defined as 50% participants who marked higher implementation scores in each or all of 5 contents. The other 50% participants group was defined as “the low implementation group (LIG)”.
The questionnaire administered before the intervention consisted of basic questions about attributes such as age and sex, the diurnal-type scale constructed by Torsvall and Åkerstedt [22] , questions on sleep habits, quality of sleep, and a Japanese version [23] of the Impact of Event Scale-Revised (IES-R) which had been usually used as PTSD scores [24] composed of 22 questions, 8 questions related to “intrusion”, 6 on “hyper-arousal” and 8 on “avoidance-numbing”. One or two months after the intervention period, the second questionnaire was administered once which consisted of questions on continuous implementation of the 5 intervention-contents and questions on the change in the consciousness to “light” and “meal” in addition to all contents of the first questionnaire. The original questions on sleep habits which Harada et al. [25] originally constructed have been used in several papers [26] -[31] .
The software used for statistical analysis was SPSS 20.0 J for Windows (SPSS Inc., Chicago, IL, USA). χ2-test was used for categorized variables and Mann-Whitney U-tests was used for ranked variables. Pearson’s correlation analysis was performed to test the relationship between two numerical variables.
2.3. Ethic Issue
The study followed the guidelines established by the Chronobiology International Journal for the conduct of research on human subjects [32] . Before administrating the questionnaires, each participant was given a written explanation that detailed the concepts and purposes of the study and stated that their answers would be used only for academic purposes. After the above explanation, all participants agreed completely with the proposal. The study was also permitted by the ethic committee in the Laboratory of Environmental Physiology, Graduate School of Integrated Arts and Sciences, Kochi University which carried out an ethical inspection of the contents of the questionnaire.
3. Results
3.1. Questionnaire Study
55 participants (20.8%) scored 25 or more can be decided to be the persons who have PTSD symptoms (Figure 2). There is no significant difference of bedtime, wake-up time, and sleep duration in weekday between HDG (High Damage Group) and LDG (Low Damage Group).
HDG participants exhibited significantly worse sleep quality than LDG participants (Mann-Whitney U-test: Z = −4.637, p < 0.001) (Figure 3). There was no significant difference in sleep latency (p > 0.05) (χ2 test: χ2-value = 0.481, df = 2, p = 0.786). HDG participants woke more frequently during sleep (Figure 4) and had more difficulty in falling asleep than LDG participants (woken during sleep: χ2-value = 48.517, df = 1, p < 0.001, difficulty in falling asleep: χ2-value = 13.378, df = 2, p = 0.001).

Figure 2. 55 participants (20.8%) scored 25 or more on IES-R. It can be decided to be the persons who have PTSD symptoms.
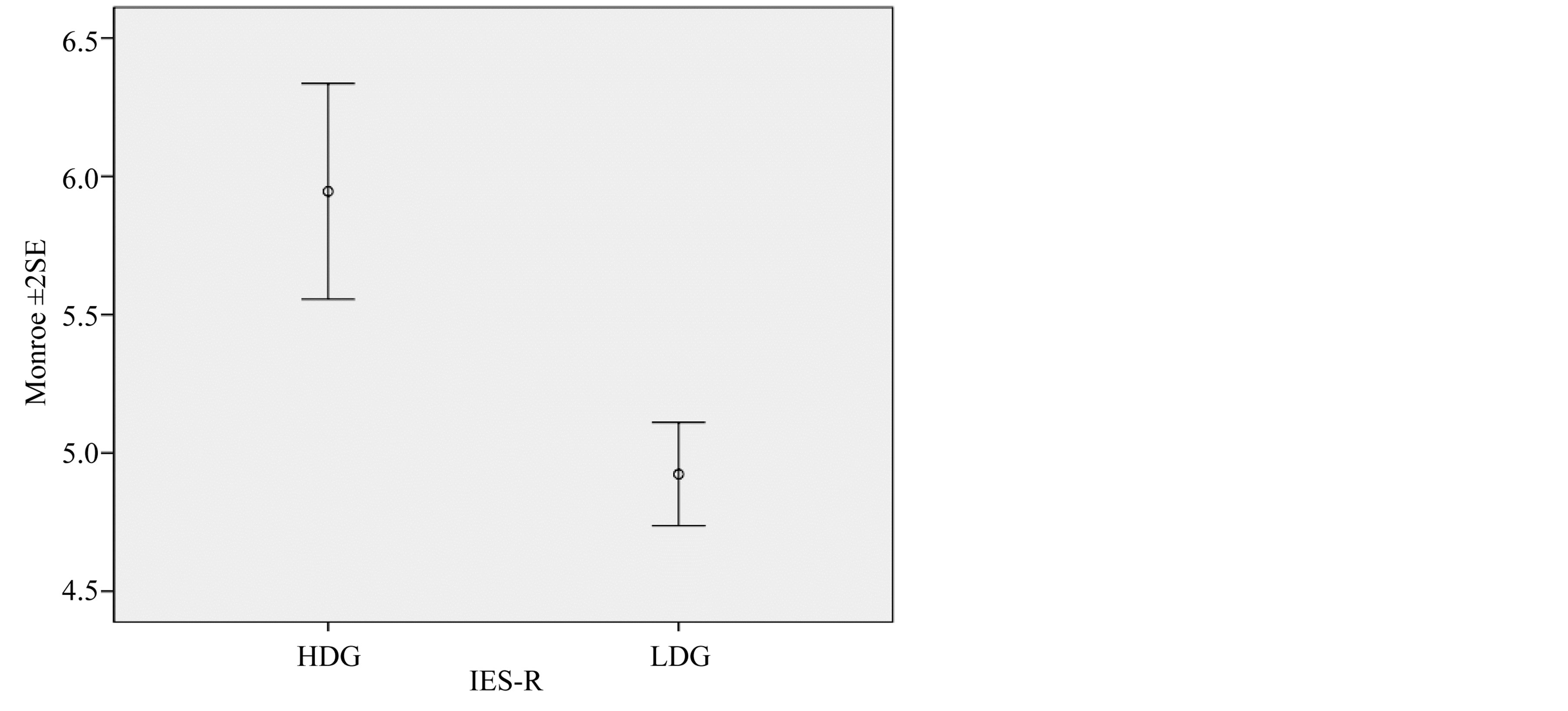
Figure 3. Comparison of current (March 2012) PTSD scores of participants of a High Damage Group (HDG) and a Low Damage Group (LDG) of the Hanshin-Awaji Great Earthquake (Jan 1995). HDG participants exhibited significantly worse sleep quality than LDG participants (Mann-Whitney U-test: Z = −4.637, p < 0.001).

Figure 4. Comparison of frequency of waking during sleep of between High Damage Group (HDG) and Low Damage Group (LDG). HDG participants woke more frequently during sleep than LDG participants (χ2 test: χ2-value = 48.517, df = 1, p < 0.001).
HDG participants exhibited significantly worse subjective sleep quality than LDG participants (Mann-Whit- ney U-test: z = −3.348, p = 0.001) (Figure 5). LDG participants fell asleep easily and slept deeply with higher frequency than HDG participants (p = 0.005, p = 0.011), although there was no difference in mood at awakening in the morning between the two groups (p > 0.05).
LDG participants tended to be more morning-typed than HDG participants (HDG: 14.17, LDG: 15.12, z = 1.659, p = 0.097) (Figure 6). Despite of degree of PTSD, significant positive correlation was shown between morning-typology and high sleep quality (HDG: DTS versus Monroe r = −0.420, p = 0.002, DTS versus Subjective QOS r = −0.580, p < 0.001; LDG: DTS versus Monroe r = −0.304, p < 0.001, ME versus Subjective QOS r = −0.359, p < 0.001).
Significant relationship of Diurnal Type Scores (DTS) didn’t appear to the IES-R score (ANOVA Variable factor: DTS score, p = 0.710), while that of Monroe’s QOS did so (Higher quality of sleep with lower IES-R score; ANOVA Variable factor: Monroe, p < 0.001).
3.2. Intervention Study
Only 1 person was over the cutoff point (between 24 and 25) before intervention (Figure 7). This high-traumatic person’s comprehensive sleep health tended to be improved through the intervention (Wilcoxon test: z = 1.941, p = 0.052) (Table 2).
The others’ (non high-traumatic persons) diurnal type scale before intervention was significantly lower (evening-type) than that after intervention (Wilcoxon test: z = 2.004, p = 0.045) (Figure 8). Sleep latency of the others was significantly shortened through the intervention (z = −2.004, p = 0.045) (Figure 9).
The wake-up time of the high implementation group on the 2nd content (Protein rich food taken at breakfast) tended to become earlier than that of the low implementation group (Mann-Whitney U-test: z = 1.807, p = 0.071). Monroe’s sleep quality index in the high implementation group on the 3rd content (Exposed to sunlight after breakfast) was significantly improved (z = 2.540, p = 0.011) and their sleep latency tended to be shorten than those of the low implementation group (z = 1.902, p = 0.057). Participants in the high implementation group on the 4th content (Cut back on the time to watch TV at night) significantly shifted morning typed than those in the low implementation group (z = −2.518, p = 0.012). Subjective sleep quality index of the high implementation group of the 5th content (Cut back on the time to be exposed to fluorescent light at night) was significantly more improved than that of the low implementation group (z = 2.159, p = 0.031) (Table 3).

Figure 5. Comparison of subjective quality of sleep index between High Damage Group (HDG) and Low Damage Group (LDG). HDG participants exhibited significantly worse sleep quality than LDG participants (Mann-Whitney U-test: z = −3.348, p = 0.001).

Figure 6. Comparison of diurnal type scale between High Damage Group (HDG) and Low Damage Group (LDG) (HDG: 14.17, LDG: 15.12, Mann-Whitney U-test: z = 1.659, p = 0.097).
4. Discussion
4.1. Questionnaire Study
In this study, 20.8% participants scored 25 or more can be decided to be the persons who have PTSD symptoms. Kun et al. [33] reported that the estimated prevalence rate of PTSD symptoms of younger adults was 28.6% (n = 364; 15 - 34 years). Their survey was conducted three months after the 2008 Sichuan earthquake. Another previous study which was undertaken 15 months after the same earthquake reported that the prevalence rate of PTSD symptoms of younger adults was 8.0% (n = 138; <60 years) [34] . In this study, estimated PTSD symptoms remain even 17 years after the Great Hanshin-Awaji Earthquake. A previous study found that PTSD became chronic in 46% of all patients who developed the disorder [35] , and Kessler et al. [36] reported that onethird of individuals who developed PTSD after traumatic event did not have remission of the disorder after ten

Figure 7. IES-R score before the intervention. Only 1 person was over the cut-off point (between 24 and 25).

Figure 8. Comparison of diurnal type scale between before and after the intervention of non high-traumatic persons who showed less than 25 of IES-R score. The diurnal type scale after intervention was significantly higher (more morningtyped) than that before the intervention (Wilcoxon test: z = 2.004, p = 0.045).

Figure 9. Comparison of sleep latency between before and after the intervention of the non high-traumatic persons. It was significantly shortened through the intervention (Wilcoxon test: z = −2.004, p = 0.045).

Table 2. Change in comprehensive variables on sleep health of the high-traumatic person with the IES-R score of 25. This sleep health of this person tended to be improved through the intervention (Wilcoxon test: z = 1.941, p = 0.052).